- Submit a Protocol
- Receive Our Alerts
- Log in
- /
- Sign up
- My Bio Page
- Edit My Profile
- Change Password
- Log Out
- EN
- EN - English
- CN - 中文
- Protocols
- Articles and Issues
- For Authors
- About
- Become a Reviewer
- EN - English
- CN - 中文
- Home
- Protocols
- Articles and Issues
- For Authors
- About
- Become a Reviewer
Vestibular Organ Dissection and Whole-Mount Immunolabeling in Mouse
Published: Vol 12, Iss 10, May 20, 2022 DOI: 10.21769/BioProtoc.4416 Views: 3071
Reviewed by: Pilar Villacampa AlcubierreOlga KopachSarajo Mohanta

Protocol Collections
Comprehensive collections of detailed, peer-reviewed protocols focusing on specific topics
Related protocols
Puromycin Proximity Ligation Assay (Puro-PLA) to Assess Local Translation in Axons From Human Neurons
Raffaella De Pace [...] Saikat Ghosh
Mar 5, 2025 3398 Views
Assay for Site-Specific Homologous Recombination Activity in Adherent Cells, Suspension Cells, and Tumor Tissues
Yuki Yoshino [...] Natsuko Chiba
Apr 5, 2025 2504 Views
Isolation and Imaging of Microvessels From Brain Tissue
Josephine K. Buff [...] Sophia M. Shi
Aug 5, 2025 2708 Views
Abstract
The vestibular sensory apparatus contained in the inner ear is a marvelous evolutionary adaptation for sensing movement in 3 dimensions and is essential for an animal’s sense of orientation in space, head movement, and balance. Damage to these systems through injury or disease can lead to vertigo, Meniere’s disease, and other disorders that are profoundly debilitating. One challenge in studying vestibular organs is their location within the boney inner ear and their small size, especially in mice, which have become an advantageous mammalian model. This protocol describes the dissection procedure of the five vestibular organs from the inner ear of adult mice, followed by immunohistochemical labeling of a whole mount preparation using antibodies to label endogenous proteins such as calretinin to label Type I hair cells or to amplify genetically expressed fluorescent proteins for confocal microscopic imaging. Using typical lab equipment and reagents, a patient technician, student, or postdoc can learn to dissect and immunolabel mouse vestibular organs to investigate their structure in health and disease.
Keywords: Inner earBackground
The vestibular system senses head movements by decomposing motion into different angular and linear directions. The three semicircular canals are oriented along horizontal and vertical planes with respect to the head and sense angular movements along their axes. The two otolith organs, the utricle and sacculus, are oriented roughly horizontally and vertically and sense linear movements in those directions. Each of the five sensory structures contain a neuroepithelium. In the base of each semicircular canal, a swelling called the crista ampularis houses the neuroepithelium. The neuroepithelium of the otolith organs are called maculae. A more general term that describes vestibular neuroepithelia is ‘end organ’. Each end organ contains hair cells whose stereocilia are embedded in a structure that is deflected by the movement of endolymph. Sensory transduction occurs at hair cells that are similar to those in the auditory system. Hair cells are mechanosensitive and release graded amounts of glutamate onto the peripheral afferents of the vestibular ganglion cells depending on the deflection of their stereocilia. The graded signal is converted to a spike rate signal by the peripheral afferents that carry it to the brain via their central-projecting axons that make up the vestibular division of the vestibulocochlear nerve. A comprehensive resource for the structure and function of the vestibular system can be found in Goldberg et al. (2012).
Immunolabeling can be used to identify specific hair cell types, such as calretinin-expressing Type I hair cells, or to localize proteins involved in mechanotransduction, cell structure, or vestibular disorders. Many publications present exemplary micrographs of whole-mounted vestibular end organs from adult mice (Li et al., 2008; Lysakowski et al., 2011; Golub et al., 2012; Spitzmaul et al., 2013; Krey et al., 2015; Bucks et al., 2017; Hoffman et al., 2018; Yoshimura et al., 2018). The purpose of this protocol is to describe the procedure in sufficient detail that others may be encouraged to study the anatomy of the vestibular system. The procedure described here was used to dissect, label, and image vestibular organs reported in Balmer and Trussell (2019).
Materials and Reagents
SecureSeal imaging spacer (Grace Bio-Labs, catalog number: SS8X9)
Superfrost Plus microscope slides (Fisher Scientific, catalog number: 12-550-15)
Coverslips #1.5 (Fisher Scientific, catalog number: 12-544-DP)
CFM-3 mounting media (Citiflour, catalog number: CFM-3)
35 mm culture dishes (Thermo Scientific, catalog number: 171099)
Paraformaldehyde (PFA) (Electron Microscopy Sciences, catalog number: 15700)
Heparin (Sigma, catalog number: H5515)
Na2HPO4 (Sigma, catalog number: S0876)
NaH2PO4 (Sigma, catalog number: S5011)
NaCl (Sigma, catalog number: S9888)
Phosphate buffered saline (PBS) (Growcells, catalog number: MRGF-6235)
Bovine serum albumin (BSA) used to coat typical 200 µL pipette tips (Sigma, catalog number: A7906)
Triton X-100 (Sigma, catalog number: X100)
Normal Donkey Serum (NDS) (Jackson ImmunoResearch, catalog number: 017-000-121)
Sylgard 184 (Fisher Scientific, catalog number: 50-366-794)
Heparinized saline (see Recipes)
4% PFA in 0.1 M PB (see Recipes)
Equipment
Dissection microscope (Zeiss, model: Stemi 305)
Fiber light (World Precision Instruments, catalog number: Z-LITE-186)
Water bath (Fisher Scientific, catalog number: S28124)
Fine forceps (Fine Science Tools, catalog number: 11254-20)
Fine curved forceps (Fine Science Tools, catalog number: 11272-30)
Laminectomy forceps (Fine Science Tools, catalog number: 11223-20)
Spring scissors (Fine Science Tools, catalog number: 15000-08)
Large scissors (Fine Science Tools, catalog number: 14101-14)
Large forceps (Fine Science Tools, catalog number: 11000-12)
Procedure
Transcardiac perfusion
Perform transcardiac perfusion with heparinized saline warmed to 37°C (see Recipe 1) until the fluid coming out of the heart runs almost clear, ~6 min.
Perfuse with 4% paraformaldehyde (PFA) in 0.1 M phosphate buffer (PB) cooled to 4°C (on ice; see Recipe 2). Perfuse ~30 mL through heart.
Note: In this protocol, this perfusion is the only fixation of the vestibular organs, so it must be done successfully. We have not found post-fixation to be necessary and were concerned that it may reduce the antigenicity of proteins during immunohistochemistry.
Brain and temporal bone extraction
Decapitate the mouse with large sharp scissors.
Using small spring scissors and forceps, carefully remove the top of the skull to expose the brain (Figure 1A–B).
Tip the brain forward and use small spring scissors to cut the vestibulocochlear nerves close to where they enter the brain (Figure 1C–D). The vestibular ganglion lies in the temporal bone at the base of the nerve, so take care not to damage it.
Note: Put the brain in 4% PFA in PBS, if retaining for histology.
The temporal bones (bulla) lie along the base of the skull on each side. Use scissors to cut them out of the base of the skull and place them PBS (Figure 1E–F).
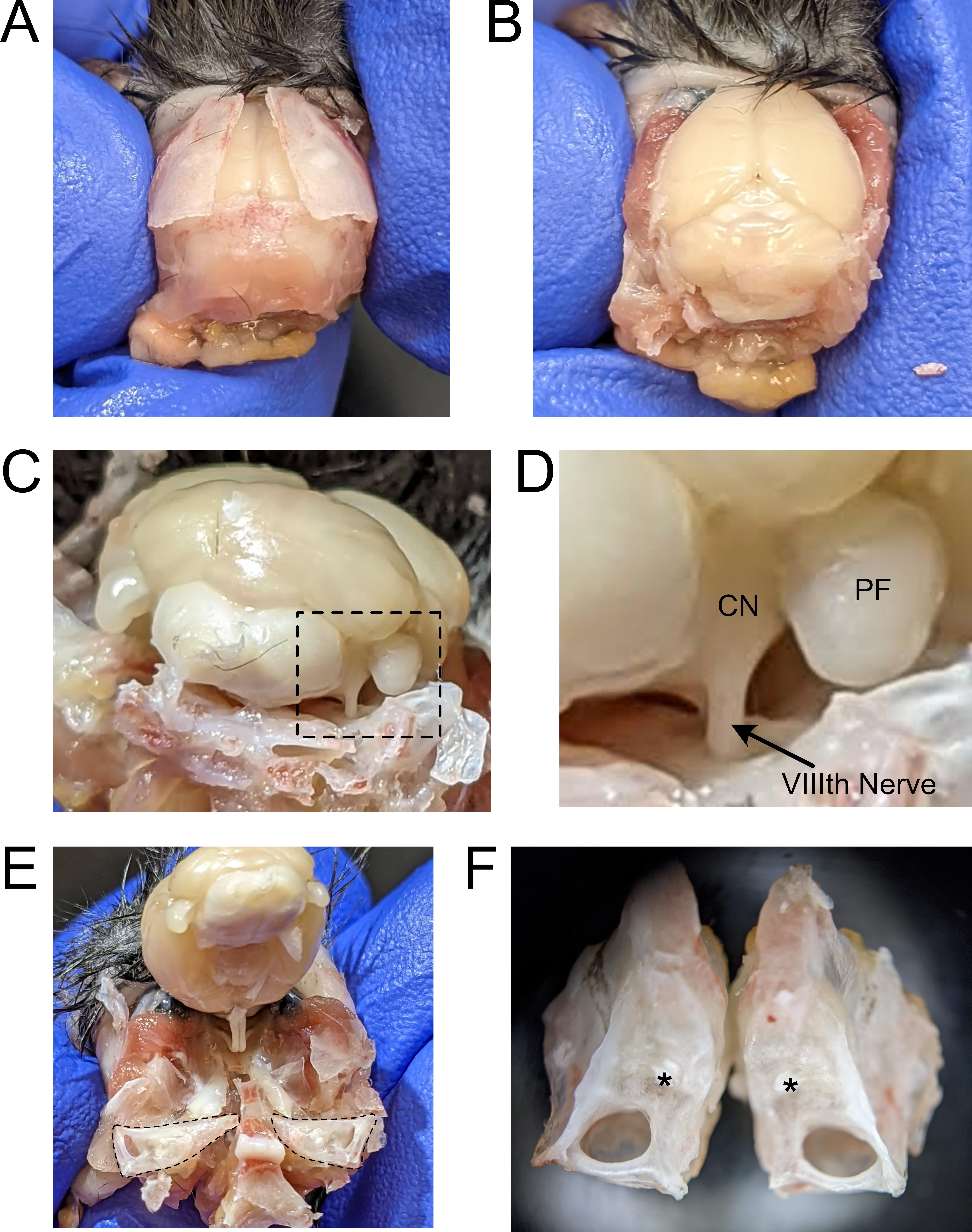
Figure 1. Brain and temporal bone extraction. A) Cuts are made along the skull sutures. B) Skull plates above the brain are removed. C) The vestibulocochlear nerve can be visualized when the skull below the brain is peeled downward. D) The vestibulocochlear nerve is cut where it enters the inner ear. CN- Cochlear Nucleus. PF- Paraflocculus. E) The temporal bones are revealed (outlined) when the brain is tipped forward and the trigeminal nerves are cut. F) Extracted temporal bones. * indicate the vestibulocochlear nerves.
Vestibular organ dissection
Place the bulla in a Sylgard 184-coated culture dish filled with PBS.
Lighting the preparation with a fiber light at various oblique angles can improve the contrast of the tissue in the dish by creating shadows.
Use large forceps to grip the entire bulla and hold it in place against the soft Sylgard on the bottom of the dish (Figure 2A).
The Sylgard prevents the bulla from sliding. Optional: A permanent marker (sharpie) can be used to darken the outside of the dish to contrast it with the light-colored end organs and bone, or an inert dye, such as India ink, can be added to the Sylgard during preparation of the dishes.
With your other hand, use fine forceps or a needle to remove the vestibular ganglion in one piece where it sits between the cochlea and labyrinths (Figure 1F). It may be difficult to tell where the vestibular ganglion is on the nerve, so it is advantageous to take out the whole nerve. Place the vestibular ganglion in a labeled 48-well plate, using a BSA-coated 200 µL pipette:
The nerve may separate into two parts, presumably the auditory and vestibular divisions. Care must be taken when removing the nerve and vestibular ganglion to avoid damaging the utricle, which is attached to the base of the nerve. Do not insert the forceps too deep into where the nerve comes through the bone, as they might damage the utricle.
Use of BSA-coated 200 µL pipette: Withdraw ~100 µL of PBS with the nerve into the pipette tip. It is optimal to keep the nerve (or end organ) suspended in solution in the pipette. It is more likely to stick to the inside of the pipette tip if it is floating at the top of the column of fluid in the tip.
Prepare 10% BSA in PBS, cut the ends off the tips to make the opening large enough to accommodate the vestibular organs (~2 mm), pipette the 10% BSA into the pipette and out several times, and then eject and let dry. Store in a petri dish to prevent dust accumulation.
Pigmented melanocytes that overlie the utricle can be visualized through the bone, which can help identify its position. Use laminectomy forceps or other stout forceps to break off small pieces of this bone, which will reveal the three vestibular end organs that are joined together- the utricle, horizontal canal crista and anterior canal crista. These may be removed together in one piece (Figure 2B–C).
On the other side of the area from which the vestibular ganglion was removed, the vertical canal end organ can be removed in a similar manner, by carefully removing the overlying bone with laminectomy forceps and then sliding fine forceps underneath it to sever the nerve and detach it from the bone (Figure 2D).
The sacculus is on the other side of the temporal bone near the cochlea and has no melanocytes, so it is difficult to see (Figure 2E). It needs to be scraped from the bone more than the other end organs, which makes the sacculus the most difficult to remove without damage.
Put all the end organs in PBS as they are removed.
It may be useful to have a picture of the vestibular system available to clarify the locations of the end organs. Keep in mind that the structures of the left and right ears are mirror images.
Practice is required to reach the skill level required to dissect all five vestibular organs without damage or loss. After becoming skilled at this procedure, time and patience remain necessary, as a careful dissection of each ear may require 30–60 min.
Best results are obtained when the dissection is followed by immunohistochemical processing on the same day.
In addition, the cochlea can be similarly removed in a few sections and processed following these guidelines.
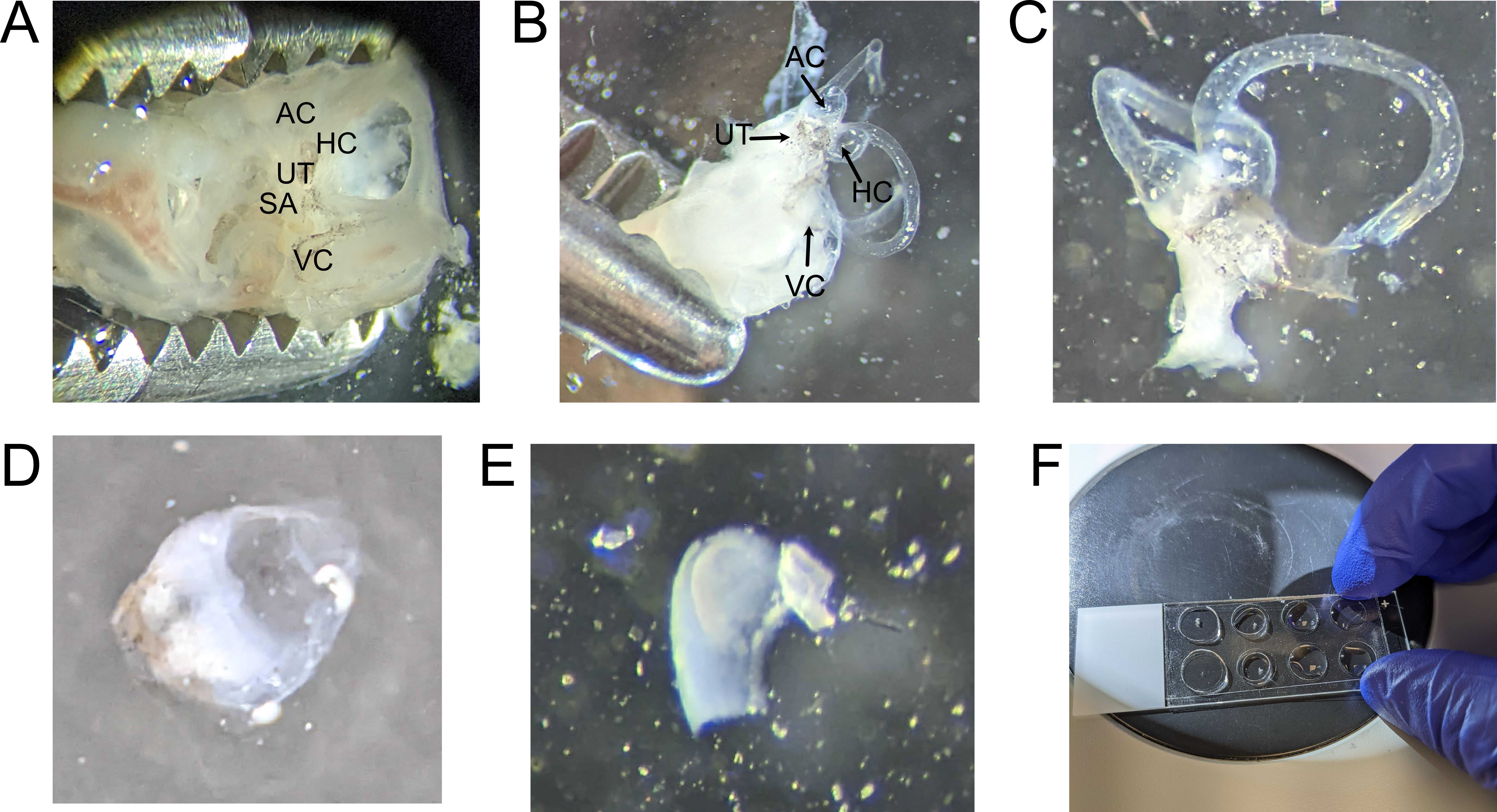
Figure 2. Vestibular organ dissection. A) The temporal bone grasped with forceps. Acronyms for the five vestibular end-organs are positioned over their locations. UT- Utricle. SA- Sacculus. AC- Anterior Canal. HC- Horizontal Canal. VC- Vertical Canal. B) After removal of some of the overlying bone, four of the vestibular end organs are revealed. C) Utricle and attached anterior canal and horizontal canal cristae. D) Dissected vertical canal crista. E) Dissected sacculus. F) Applying a coverslip to the vestibular organs positioned within the spacer.
Immunohistochemistry of vestibular end organs
To transfer the end organs during rinses, etc., use a BSA-coated 200 µL pipette tip, as described above. Transfer the end organs to a different well in the 48-well plate containing the new solution (at least 200 µL in a 48-well plate).
Moving all of the end organs down one row may help keep them organized.
The previous solution that is transferred with the end organ in the pipette should be as small in volume as possible. A gentle flick may be necessary to cause the end organ to fall to the bottom of the column of solution that is suspended in the pipette tip and can then be ejected with minimal fluid.
Permeabilize and block in 2% Triton X-100, 5% NDS 1 h room temperature on an orbital shaker.
This high concentration of detergent may be necessary for optimal staining of this preparation.
Remove the end organs from the permeabilization and blocking buffer and place in primary antibody diluted in 5% NDS. Incubate in primary antibody overnight on an orbital shaker at 4 °C (Table 1). Incubation for up to 3 days may enhance antibody penetration.
We avoid rinsing between these steps as each transfer of the end organs represents a risk of damage or loss.
Table 1. Primary antibodies
Antibody Source Concentration Rabbit polyclonal anti-calretinin Swant, 7697 1:500 Chicken polyclonal anti-GFP Aves Labs, GFP-1020 1:500 Goat polyclonal anti-mCherry Sicgen, AB0040-200 1:500
Rinse 3 × 10 min in PBS by removing end organs from primary and placing into a different well in the 48-well plate containing fresh PBS.
Transfer end organs into secondary antibodies diluted in 5% NDS and incubate overnight 4°C on orbital shaker (Table 2).
Table 2. Secondary antibodies
Antibody Source Concentration Donkey polyclonal anti-rabbit Cy3 Jackson ImmunoResearch Labs, 711-165-152 1:500 Donkey polyclonal anti-chicken Alexa Fluor 488 Jackson ImmunoResearch Labs, 703-545-155 1:500 Donkey polyclonal anti-goat Cy3 Jackson ImmunoResearch Labs, 705-165-147 1:500 Rinse 3 × 10 min in PBS by removing end organs from primary and placing into a different well in the 48-well plate containing fresh PBS.
Mounting and coverslipping
Place an 8-well 120 µm thick spacer onto a microscope slide (SecureSeal): First remove the plastic side and put the spacer on the slide. Flatten it down by running a flat object along it, taking care to not contaminate the glass of the microscope slide. Then, remove the paper side. It will be sticky from now until the coverslip is placed over it, so be extremely careful to avoid accidentally touching it. In our experience, this is preferred over trying to remove the paper and expose the adhesive after laying out all the end organs as their positioning is easily disrupted. Alternatively, each end organ can be placed on a separate slide with a single well spacer.
Place one end organ on the slide within the spacer in a pool of PBS. Using fine forceps, remove the melanocytes or any membranes that would be between the coverslip and the face of the end organ. The canal cristae typically lie on their side, which is optimal for imaging. The utricle and sacculus can be laid such that the nerve is against the microscope slide with the hair cell side pointing upward toward the coverslip. This step is critical for good imaging. Apply more PBS so that it does not dry out while mounting the others, but not so much that it is free to float away from the microscope slide. Repeat for each end organ and the vestibular ganglion or nerve in separate wells of the spacer.
Ensure that all the end organs are oriented properly, and then remove excess PBS with a normal 200 µL pipette tip (unmodified). Let it dry slightly so that they stick to the positively charged Superfrost Plus microscope slides.
Apply a generous amount of CFM-3 mounting media to each well. Apply coverslip to the adhesive SecureSeal spacer (Figure 2F).
Notes:
It is far better for excess media to flow out when applying the coverslip than for air bubbles to be trapped in the wells; apply ample mountant.
Note that repositioning of the coverslip is nearly impossible due to the adhesive face of the SecureSeal spacer, so apply it carefully.
Confocal imaging
This preparation can be imaged with typical confocal imaging described elsewhere. Long-working distance objectives may be necessary to image through the entire end organ and underlying nerve. We used a Zeiss 25× 0.8 NA oil immersion objective on a Zeiss LSM 880 for full end organ imaging (Figure 3). For imaging of smaller areas, we used a Zeiss 63× 1.4 NA oil immersion objective (Figure 4).
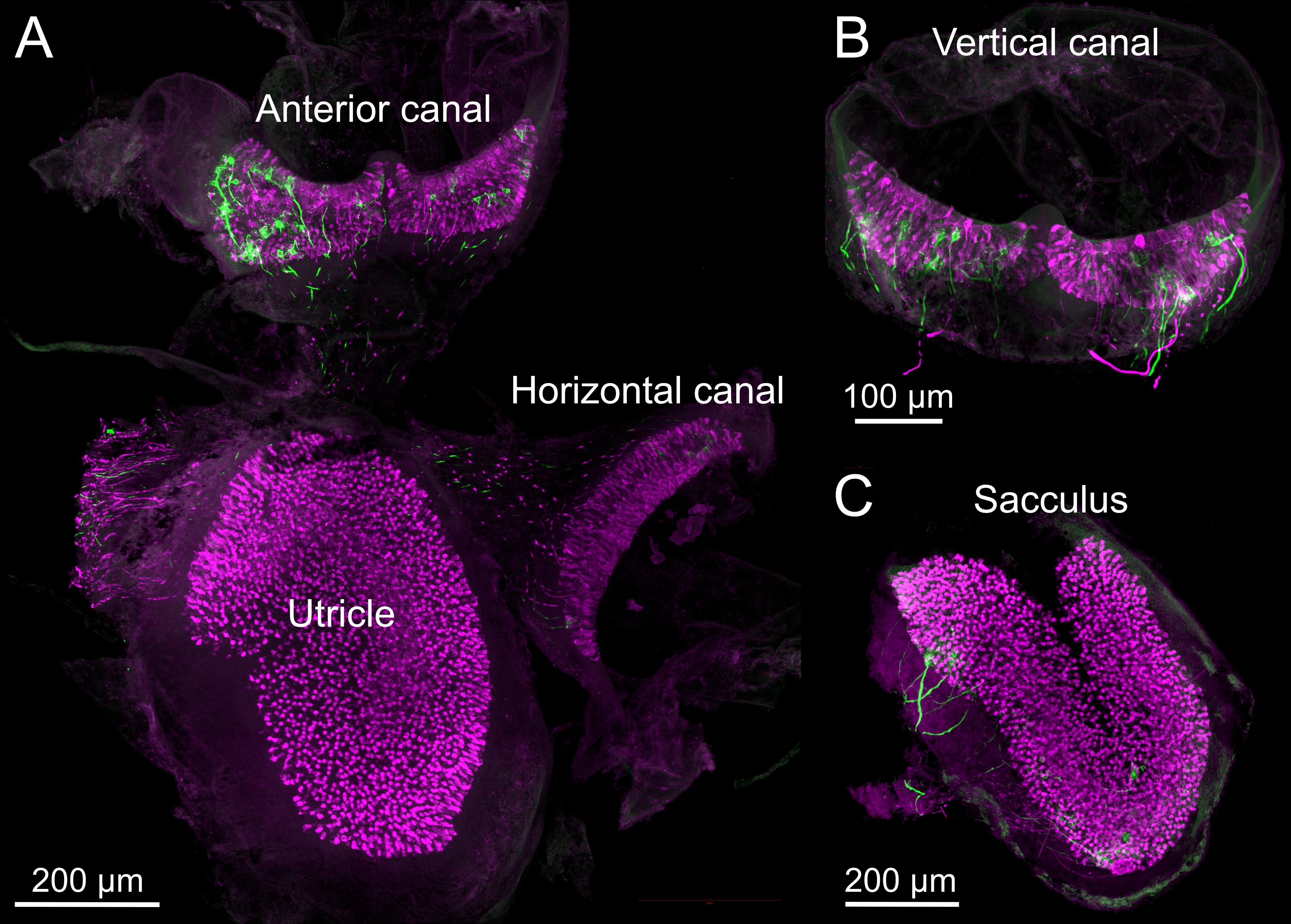
Figure 3. Vestibular end organ whole mounts imaged with 25× objective. A) The utricular macula, anterior canal crista, and horizontal canal crista can be dissected out of the temporal bone in one piece. Calretinin (magenta) is expressed in Type I hair cells. Single nerve fibers are labeled with green fluorescent protein (GFP) that has been amplified with Alexa Fluor 488. B-C) The vertical canal (B) and sacculus (C) are separated during the dissection and are therefore processed and mounted separately.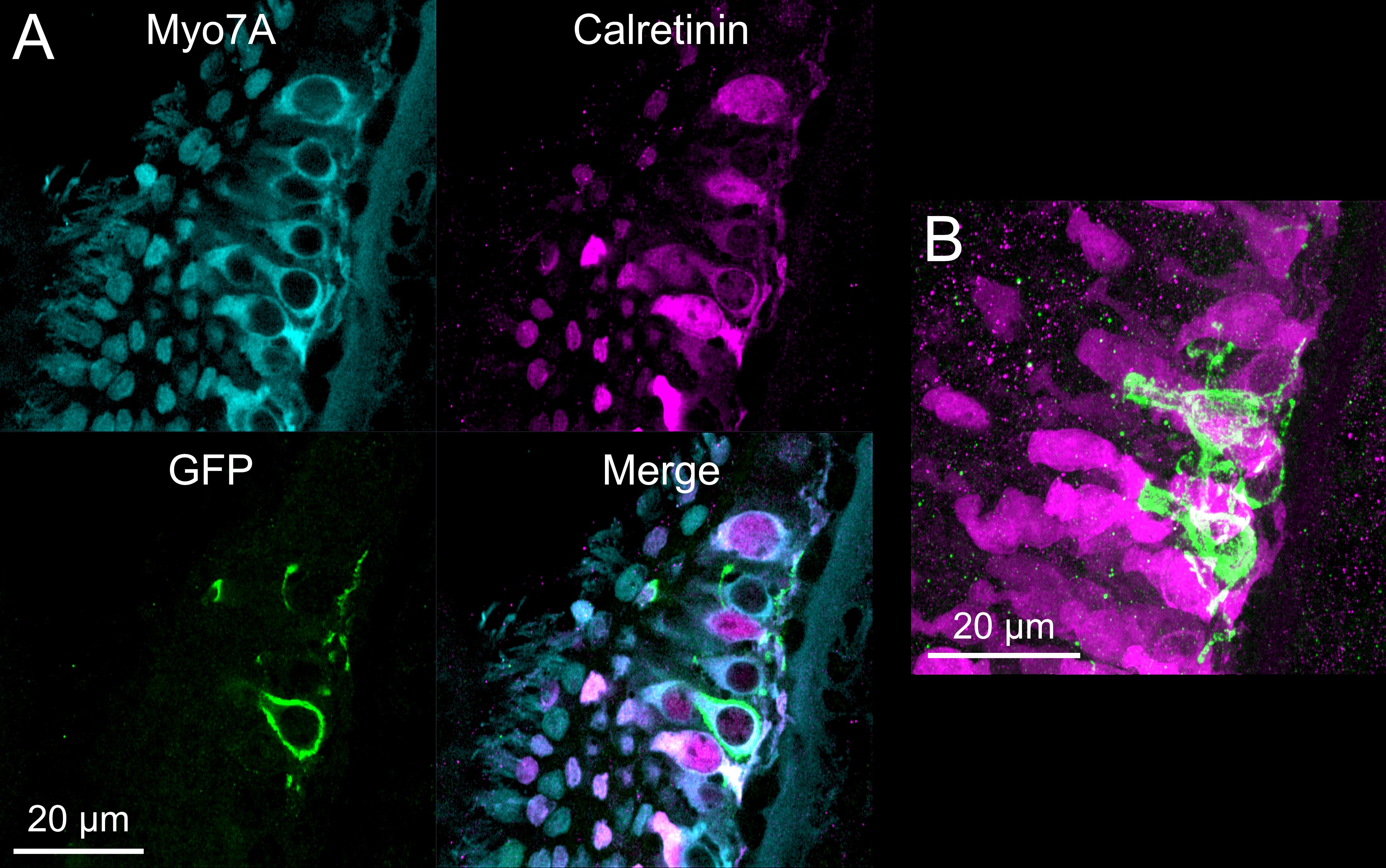
Figure 4. Vestibular hair cells and peripheral vestibular afferents imaged with 63× objective. A) Single optical plane showing Myo7A (cyan), present in all hair cells; calretinin (magenta), present in Type I hair cells; GFP (green), expressed by an retrograde-AAV injected into the cerebellum and amplified with an anti-GFP antibody; and merged image showing that the retrolabeled peripheral afferent is a flask shape and surrounds a calretinin expressing hair cell. B) Maximum intensity projection of 24 µm thick image stack showing calretinin (magenta) and GFP (green).
Recipes
Heparinized saline
Add 3.6 g NaCl, 0.022 g heparin (calculated to be 10 U/mL final concentration), and 400 mL of dH2O
4% PFA in 0.1 M PB
Add 10 mL of 16% PFA, 6.2 mL of 0.5 M Na2HPO4, 0.9 mL of 1 M NaH2PO4, and raise to 40 mL with dH2O
Acknowledgments
We thank Drs. Jocelyn Krey and Peter Barr-Gillespie for their expertise in this procedure and inner ear anatomy. Funding was provided by NIH F32 DC014878, NIH K99 DC016905, and Hearing Health Foundation Emerging Research Grants to TSB, NIH R01 NS028901, NIH RO1 DC004450 to LOT, and NIH P30 NS0618000 to S Aicher. This protocol was derived from Balmer and Trussell (2019).
Competing interests
The authors declare no competing interests.
Ethics
All procedures were approved by the Oregon Health and Science University’s Institutional Animal Care and Use Committee and met the recommendations of the Society for Neuroscience.
References
- Balmer, T. S. and Trussell, L. O. (2019). Selective targeting of unipolar brush cell subtypes by cerebellar mossy fibers. Elife 8: e44964.
- Bucks, S. A., Cox, B. C., Vlosich, B. A., Manning, J. P., Nguyen, T. B. and Stone, J. S. (2017). Supporting cells remove and replace sensory receptor hair cells in a balance organ of adult mice. Elife 6: e18128.
- Goldberg, J. M., Wilson, V. J., Cullen, K. E., Angelaki, D. E., Broussard, D. M., Buttner-Ennever, J., Fukushima, K. and Minor, L. B. (2012). The Vestibular System: A Sixth Sense. New York: Oxford University Press. Available at: https://oxford.universitypressscholarship.com/10.1093/ acprof:oso/9780195167085.001.0001/acprof-9780195167085 [Accessed November 24, 2021].
- Golub, J. S., Tong, L., Ngyuen, T. B., Hume, C. R., Palmiter, R. D., Rubel, E. W. and Stone, J. S. (2012). Hair cell replacement in adult mouse utricles after targeted ablation of hair cells with diphtheria toxin. J Neurosci 32(43): 15093-15105.
- Hoffman, L. F., Choy, K. R., Sultemeier, D. R. and Simmons, D. D. (2018). Oncomodulin Expression Reveals New Insights into the Cellular Organization of the Murine Utricle Striola. J Assoc Res Otolaryngol 19(1): 33-51.
- Krey, J. F., Sherman, N. E., Jeffery, E. D., Choi, D. and Barr-Gillespie, P. G. (2015). The proteome of mouse vestibular hair bundles over development. Scientific Data 2(1): 150047.
- Li, A., Xue, J. and Peterson, E. H. (2008). Architecture of the mouse utricle: macular organization and hair bundle heights. J Neurophysiol 99(2): 718-733.
- Lysakowski, A., Gaboyard-Niay, S., Calin-Jageman, I., Chatlani, S., Price, S. D. and Eatock, R. A. (2011). Molecular microdomains in a sensory terminal, the vestibular calyx ending. J Neurosci 31(27): 10101-10114.
- Spitzmaul, G., Tolosa, L., Winkelman, B. H., Heidenreich, M., Frens, M. A., Chabbert, C., de Zeeuw, C. I. and Jentsch, T. J. (2013). Vestibular role of KCNQ4 and KCNQ5 K+ channels revealed by mouse models. J Biol Chem 288(13): 9334-9344.
- Yoshimura, H., Shibata, S. B., Ranum, P. T. and Smith, R. J. H. (2018). Enhanced viral-mediated cochlear gene delivery in adult mice by combining canal fenestration with round window membrane inoculation. Sci Rep 8(1): 2980.
Article Information
Copyright
Balmer and Trussell. This article is distributed under the terms of the Creative Commons Attribution License (CC BY 4.0).
How to cite
Readers should cite both the Bio-protocol article and the original research article where this protocol was used:
- Balmer, T. S. and Trussell, L. O. (2022). Vestibular Organ Dissection and Whole-Mount Immunolabeling in Mouse. Bio-protocol 12(10): e4416. DOI: 10.21769/BioProtoc.4416.
- Balmer, T. S. and Trussell, L. O. (2019). Selective targeting of unipolar brush cell subtypes by cerebellar mossy fibers. Elife 8: e44964.
Category
Neuroscience > Peripheral nervous system
Neuroscience > Sensory and motor systems
Cell Biology > Tissue analysis > Tissue isolation
Do you have any questions about this protocol?
Post your question to gather feedback from the community. We will also invite the authors of this article to respond.
Share
Bluesky
X
Copy link









