- Submit a Protocol
- Receive Our Alerts
- Log in
- /
- Sign up
- My Bio Page
- Edit My Profile
- Change Password
- Log Out
- EN
- EN - English
- CN - 中文
- Protocols
- Articles and Issues
- For Authors
- About
- Become a Reviewer
- EN - English
- CN - 中文
- Home
- Protocols
- Articles and Issues
- For Authors
- About
- Become a Reviewer
Candida Biofilm Formation Assay on Essential Oil Coated Silicone Rubber
Published: Vol 11, Iss 5, Mar 5, 2021 DOI: 10.21769/BioProtoc.3941 Views: 3681
Reviewed by: Alba BlesaDevanshi D KhokhaniTimo A Lehti

Protocol Collections
Comprehensive collections of detailed, peer-reviewed protocols focusing on specific topics
Related protocols

A Simple and Reproducible Stereomicroscopic Method to Assess Fungal Biofilms: Application to Antifungal Susceptibility Testing
Zinnat Shahina and Tanya E. S. Dahms
Jul 5, 2023 1670 Views
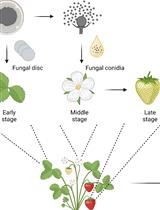
Botrytis cinerea in vivo Inoculation Assays for Early-, Middle- and Late-stage Strawberries
Piao Yang [...] Ye Xia
Oct 20, 2023 2829 Views

In Vitro Hyphal Branching Assay Using Rhizophagus irregularis
Takaya Tominaga and Hironori Kaminaka
Aug 20, 2024 2387 Views
Abstract
Development of biofilm associated candidemia for patients with implanted biomaterials causes an urgency to develop antimicrobial and biofilm inhibitive coatings in the management of recalcitrant Candida infections. Recently, there is an increase in the number of patients with biofilm formation and resistance to antifungal therapy. Therefore, there is a growing interest to use essential oils as coating agents in order to prevent biomaterial-associated Candida infections. Often high costs, complicated and laborious technologies are used for both applying the coating and determination of the antibiofilm effects hampering a rapid screening of essential oils. In order to determine biofilm formation of Candida on essential oil coated surfaces easier, cheaper and faster, we developed an essential oil (lemongrass oil) coated surface (silicone-rubber) by using a hypromellose ointment/essential oil mixture. Furthermore, we modified the “crystal violet binding assay” to quantify the biofilm mass of Candida biofilm formed on the lemongrass oil coated silicone rubber surface. The essential oil coating and the biomass determination of biofilms on silicone rubber can be easily applied with simple and accessible equipment, and will therefore provide rapid information about whether or not a particular essential oil is antiseptic, also when it is used as a coating agent.
Keywords: Biofilm formationBackground
In recent years, the frequency of Candida infections caused by both nosocomial and opportunistic Candida strains has increased rapidly especially due to the growing number of transplant recipients, cancer patients and patients who receive immunosuppressive therapy (Sanguinetti et al., 2015). Apart from this, development of candidemia in patients with implanted biomaterials such as catheters (Simitsopoulou et al., 2014), dental implants (Li et al., 2012), voice prostheses (Talpaert et al., 2015) and prosthetic devices (Ramage et al., 2006) causes an urgency to develop preventive strategies such as antimicrobial coatings in the management of recalcitrant Candida infections (Ramage et al., 2006). Since biofilm formation plays a pivotal role in the development of recalcitrant candidemia (Simitsopoulou et al., 2014), not only antimicrobial therapies, but also antibiofilm strategies are needed for the prevention of biomaterial-associated Candida infections. Recently, a growing increase in the incidence of candidemia has been associated with the increase in biofilm formation and resistance to antifungal therapy (Francisconi et al., 2020). Substances obtained from traditional medicinal plants, such as volatile essential oils have been regarded as attractive sources for new antimicrobials(Francisconi et al., 2020). Essential oils, originating from different parts of a variety of aromatic plants not only have antimicrobial but also have antibiofilm effects against various microorganisms (Akthar et al., 2014; Kim et al., 2016; Sahal et al., 2019 and 2020). Therefore, the antibiofilm effects of several essential oils against different Candida species have been studied for years (Almeida et al., 2016; Kryvtsova et al., 2019). Recently, essential oils have also been evaluated as agents that prevent biomaterial-associated Candida infections. In particular, there is a growing interest in the use of a lemongrass essential oil as a coating agent (Sahal et al., 2019 and 2020). Often high costs and complicated technologies are used for both applying the coating and determination of the antibiofilm effects. For example, Liakos et al. (2017) used electrospinning to apply a cellulose acetate based coating containing the essential oil and Anghel et al. (2012) used Confocal Laser Scanning Microscopy images to asses fungal biofilm architecture on Fe3O4/C18/essential oil coated ProvoxTM voice prostheses. These techniques are often very expensive, laborious and require highly qualified equipment and personnel. Thus, they constrain an ease and rapid screening of essential oils. Therefore, we aimed to develop cheap, effective and easily applicable protocols to rapidly screen the anti-candida biofilm effects of various essential oils coated on silicone rubber.
In the first part, we describe the preparation of essential oil coated silicone rubber surface using a hypromellose ointment/essential oil mixture. In this part, hypromellose ointment was used as a vehicle because it mixes well with essential oils and because of its good adhesive properties to wetted surfaces. In the second part, we describe the determination of the biofilm mass of Candida biofilm on these surfaces using a modified crystal violet binding assay. Both protocols can be applied easily and rapidly with simple and accessible equipment.
Materials and Reagents
VST Silicone elastomer (low viscosity, translucent silicone) (10 × 10 × 1.5 mm sheets) (Polymerization conditions: 5-bar pressure, 45 °C, 90 min.) (Maxillofacial Silicone System, Technovent Ltd., South Wales, UK, catalog number: VST-50HD Shore A 38, cure time overnight).
Petri dish (90 mm × 17 mm) (Isolab, catalog number: 0 8102061 )
Erlenmayer Flask (250 ml) (Isolab, catalog number: 027.01.250 )
6-Well plates (Biofil, catalog number: TCP 011006 )
24-Well plates (Biofil, catalog number: TCP 011024 )
Centrifugal tube 50 ml (Orange Scientific, catalog number: 4440100N )
Candida strains (Clinical Candida isolates, previously characterized as highly biofilm forming and identified using the 18S Ribosomal RNA Gene Sequence Analysis; or biofilm-positive ATCC Candida strains such as Candida albicans (Robin) Berkhout (ATCC®, catalog number: MYA-274 MYA-274TM )
Lemongrass essential oil (Merck, catalog number: 0 5521501 )
Hypromellose ointment [Hypromellose 4000 mPa.s 20% (w/w); Soft paraffin white 80% (w/w)], [FNA (Formularium der Nederlandse Apothekers), Dutch Pharmacists' Formulary, 2013], (Fagron, catalog number: 102064 )
Crystal Violet Powder (Merck, catalog number: C0775-100G )
Brain Heart Infusion (BHI) Powder (Merck, catalog number: M110493.0500 )
Agar-agar (Merck, catalog number: M101613.0500 )
Ethanol 96% (v/v) (Isolab, catalog number: 9200262500 )
Extran MA 02 (Merck, catalog number: 107553 )
K2HPO4 (Merck, catalog number: 7758-11-4)
KH2PO4 (Merck, catalog number: 7778-77-0 )
Distilled Water
Brain Heart Infusion Broth (see Recipes)
Brain Heart Infusion Agar (see Recipes)
1% Crystal Violet Solution (see Recipes)
10 mM Potassium phosphate buffer (see Recipes)
Equipment
Bunsen burner
Porcelain mortar [Outside diameter 10.5 cm, inner diameter 9.0 cm, inner depth 4.5 cm. Content 100 ml. Glazed to grinding surface, grinding surface unglazed and porcelain pestle (Length 11 cm, unglazed on grinding surface, further glazed)] (Haldenwanger, Berlin)
Forceps
Spectrophotometer (UV-Visible Spectrophotometer; Shimadzu, model: UV-1700, catalog number: 206-98366A )
Centrifuge (Eppendorf, model: 5810R, with an Eppendorf Swing-bucket rotor A-4-62 , catalog number: 5810000327)
pH Meter (ConsortTM C3010 Benchtop Multiparameter Analyzer) (Fisher Scientific, catalog number: 11772009 )
Thoma Counting Chamber (Neubauer, catalog number: C964110 )
Autoclave (Priorclave, Catalog number: 12758935 )
Light Microscope (LEICA, model: DM500 )
Incubator (Static) (Dedeoglu, catalog number: MMF-KM-068 )
Software
MINITAB (Version 18)
ImageJ (Version 1.49)
Procedure
Preparation of essential oil coated silicone rubber surfaces by using hypromellose ointment (see also Figure 1)
Mix hypromellose ointment with a particular essential oil (w/w) under aseptic conditions using a sterile porcelain mortar and pestle.
Place a layer of essential oil/hypromellose ointment mixture (50 mg) (w/w) in a sterile Petri dish under sterile conditions by using a Bunsen burner.
Clean silicone rubber surface sheets by rinsing them with 2% Extran MA02 in water followed by tap water, 70% ethanol solution (v/v) and sterile demineralized water.
Place the sterile silicone rubber surface sheet (10 × 10 mm) on top of a layer of essential oil/hypromellose ointment mixture (w/w).
Apply a gentle pressure onto the silicone rubber surface sheet to let the essential oil/hypromellose ointment mixture stick onto the material.
Take essential oil coated silicone rubber surface sheet gently out of the Petri dish by using sterile forceps and place it in a well of a sterile 6-Well plate for the further analysis.
Place the essential oil coated silicone rubber surface sheet vertical on a sterile Petri dish and put them under a light microscope (×10) in order to capture an image that contains thicknesses of both the silicone rubber sheet and the coating.
Set the thickness of the silicone rubber sheet as 1.5 mm and estimate the thickness of the essential oil/hypromellose ointment coatings on the silicone rubber surfaces by using ImageJ Software.

Figure 1. Preparation of essential oil coated silicone rubber by using essential oil/hypromellose ointment mixture. A. Placement of essential oil/hypromellose ointment mixture in a sterile Petri dish. B. Placement of a sterile biomaterial surface sheet on top of a layer of essential oil/hypromellose ointment mixture and application of a gentle pressure onto the biomaterial surface sheet to let the essential oil/hypromellose ointment mixture stick onto the material. C. Taking essential oil coated surface sheet gently out of the Petri dish.
Determination of Candida biofilm formation on essential oil coated surfaces (see also Figure 2)
Inoculate Candida strains from stock culture (grown in BHI with glycerol) into Brain Heart Infusion (BHI) agar by a streak plating technique and incubate them for 24 h at 37 °C under aerobic conditions.
Inoculate single colonies of Candida strains for pre-culture preparations into 10 ml BHI broth and incubate overnight at 37 °C without shaking.
Inoculate 10 ml preculture into the 200 ml BHI broth and grow it for 24 h at 37 °C without shaking to obtain main culture.
Harvest Candida cells by centrifugation at 3,220 × g for 10 min at 5 °C and wash 3 times with 30 ml 10 mM potassium phosphate buffer (pH 7.0).
Count Candida cells that exist in 8 different medium squares of a Thoma Counting Chamber under a light microscope with 40× objective. Calculate the average of the cells for a single medium square and calculate the Candida cell density considering the volume of a single medium square of the Thoma Counting Chamber. Adjust cell density to 3 × 106 cells/ml in BHI broth.
Place the essential oil coated silicone rubber surfaces, silicone rubber surfaces with only hypromellose ointment and the silicone rubber surfaces without any coating (positive controls) into the wells of a 24-well plate.
Add 2 ml of Candida suspensions to the wells of 24-well plates that include the different silicone rubber surfaces and incubate them for 7 days at 37 °C under aerobic conditions without shaking.
After 7 days of incubation, wash gently three times the materials harboring biofilm with 10 mM potassium phosphate buffer (pH 7) and stain them with a 1% (w/v) solution of crystal violet in sterile distilled water for 20 min at 25 °C.
Subsequently, gently rinse the materials with 10 mM potassium phosphate buffer (pH 7.0) again until no crystal violet residue left in the washing solution.
Dissolve crystal violet bound to the biofilm on the different tested surfaces in 2 ml ethanol (96%; v/v) for 20 min (O’Toole, 2011).
Measure the absorbance of dissolved crystal violet at 560 nm using a spectrophotometer (O’Toole, 2011).

Figure 2. Biofilm formation of Candida. Images of A) silicone rubber surface B) Biofilm formation on 8% Lemongrass oil coated silicone rubber surface C) Biofilm formation on 0% Lemongrass oil coated silicone rubber surface (hypromellose ointment alone) D) Biofilm formation on silicone rubber without coating (positive control).
Data analysis
Set the absorbance value of the silicone rubber surface without any coating and microorganism, but following the same procedure as the biofilm growth and crystal violet staining, as a negative control. Subtract this value from the absorbance values of the surfaces with biofilms.
Evaluate biofilm formation on the silicone rubber surface without coating as a positive control and set it as 100%. Set silicone rubber surface coated with hypromellose ointment without any essential oil as 0% essential oil coated surface.
Measure the absorbance values of biofilm formations of treatments and calculate decrease (%) in biofilm formation of treatments relative to the positive control, using the equation:
% Decrease = [(Absorbance Positive Control (560 nm) – Absorbance Treatment (560 nm))/Absorbance Positive Control (560 nm)] × 100%
Perform statistical analysis using MINITAB 18 software.
Apply Anderson-Darling test to determine if biofilm formation and biofilm inhibition data were normally distributed. Following this, apply Levene's test to assess homogeneity of variances.
In case the results are found to be normally distributed, apply two factor experimental design and do pairwise comparisons by the Tukey test. In case the results are not found as normally distributed, use non-parametric tests (Kruskal-Wallis and Mann-Whitney U tests) to evaluate the results.
Notes
Determination of biofilm formation of Candida on essential oil coated silicone rubber surfaces by modified crystal violet binding assay need to be performed at least in triplicate, including controls.
When the absorbance is too high, dilute the dissolved crystal violet and multiply the absorbance value by the dilution factor.
Recipes
Brain Heart Infusion Broth (1 L)
Dissolve 37 g BHI powder in 1 L distilled water and sterilize the medium at 121 °C for 15 min using an autoclave.
Brain Heart Infusion Agar (1 L)
Dissolve 37 g BHI powder and 30 g Agar-Agar powder in 1 L distilled water and place the media into sterile Petri dishes after sterilization at 121 °C for 15 min using an autoclave.
1% Crystal Violet Solution (w/v)
Dissolve 5 g crystal violet in 500 ml distilled water and incubate the crystal violet solution (1%, w/v) in shaking incubator for 2 h at 150 rpm, at room temperature.
10 mM Potassium Phosphate Buffer (pH 7.0) (1 L)
Dissolve 4.35 g K2HPO4 and 3.4 g KH2PO4 in 100 ml distilled water to obtain stock 0.5 M Potassium Phosphate Buffer.
Dilute 0.5 M potassium phosphate buffer to 10 mM potassium phosphate buffer.
Adjust the pH of the buffer to 7.0 by using pH meter and sterilize the buffer at 121 °C for 15 min using an autoclave.
Acknowledgments
This study was supported by funding received from Scientific Research Projects Coordination Unit (grant number: FDK-2016-10821) of Hacettepe University, Ankara, Turkey. This protocol was derived from Sahal et al. (2020).
Competing interests
The authors declare no competing financial interests.
References
- Akthar, M. S., Degaga, B. and Azam, T. (2014). Antimicrobial activity of essential oils extracted from medicinal plants against the pathogenic microorganisms : A review. Biol Sci Pharm Res 2(1): 1-7.
- Almeida, Lde, F., Paula, J. F., Almeida, R. V., Williams, D. W., Hebling, J. and Cavalcanti, Y. W. (2016). Efficacy of citronella and cinnamon essential oils on Candida albicans biofilms. Acta Odontol Scand 74(5): 393-398.
- Anghel, I., Grumezescu, V., Andronescu E., Anghel G. A. Grumezescu, A. M., Mihaiescu, D. E. and Chifiriuc M. C. (2012). Protective effect of magnetite nanoparticle/Salvia officinalis essential oil hybrid nanobiosystem against fungal colonization on the Provox® voice section prosthesis. Dig J Nanomater Biostructures 7(3): 1205-1212.
- Francisconi, R. S., Huacho, P. M. M., Tonon, C. C., Bordini, E. A. F., Correia, M. F., Sardi, J. C. O. and Spolidorio, D. M. P. (2020). Antibiofilm efficacy of tea tree oil and of its main component terpinen-4-ol against Candida albicans. Braz Oral Res 34: e050.
- Kim, Y. G., Lee, J. H., Gwon, G., Kim, S. I., Park, J. G. and Lee, J. (2016). Essential Oils and Eugenols Inhibit Biofilm Formation and the Virulence of Escherichia coli O157:H7.Sci Rep 6: 36377.
- Kryvtsova, M. V., Salamon, I., Koscova, J., Bucko, D. and Spivak, M. (2019). Antimicrobial, antibiofilm and biochemichal properties of Thymus vulgaris essential oil against clinical isolates of opportunistic infections. Biosyst Divers 27(3): 270-275.
- Li, J., Hirota, K., Goto, T., Yumoto, H., Miyake, Y. and Ichikawa, T. (2012). Biofilm formation of Candida albicans on implant overdenture materials and its removal. J Dent 40(8): 686-692.
- Liakos, I. L., Holban, A. M., Carzino, R., Lauciello, S. and Grumezescu, A. M. (2017). Electrospun Fiber Pads of Cellulose Acetate and Essential Oils with Antimicrobial Activity. Nanomaterials (Basel) 7(4): 84.
- O'Toole, G. A. (2011). Microtiter dish biofilm formation assay. J Vis Exp 47: 2437.
- Ramage, G., Martinez, J. P. and Lopez-Ribot, J. L. (2006). Candida biofilms on implanted biomaterials: a clinically significant problem. FEMS Yeast Res 6(7): 979-986.
- Sahal, G., Woerdenbag, H. J., Hinrichs, W. L. J., Visser, A., Tepper, P. G., Quax, W. J., van der Mei, H. C. and Bilkay, I. S. (2020). Antifungal and biofilm inhibitory effect of Cymbopogon citratus (lemongrass) essential oil on biofilm forming by Candida tropicalis isolates; an in vitro study. J Ethnopharmacol 246: 112188.
- Sahal, G., Nasseri, B., Ebrahimi, A. and Bilkay, I. S. (2019). Electrospun essential oil-polycaprolactone nanofibers as antibiofilm surfaces against clinical Candidatropicalis isolates. Biotechnol Lett 41(4-5): 511-522.
- Sanguinetti, M., Posteraro, B. and Lass-Florl, C. (2015). Antifungal drug resistance among Candida species: mechanisms and clinical impact. Mycoses 58 Suppl 2: 2-13.
- Simitsopoulou, M., Kyrpitzi, D., Velegraki, A., Walsh, T. J. and Roilides, E. (2014). Caspofungin at catheter lock concentrations eradicates mature biofilms of Candida lusitaniae and Candida guilliermondii. Antimicrob Agents Chemother 58(8): 4953-4956.
- Talpaert, M. J., Balfour, A., Stevens, S., Baker, M., Muhlschlegel, F. A. and Gourlay, C. W. (2015). Candida biofilm formation on voice prostheses. J Med Microbiol 64(Pt 3): 199-208.
Article Information
Copyright
© 2021 The Authors; exclusive licensee Bio-protocol LLC.
How to cite
Sahal, G., Woerdenbag, H. J., Hinrichs, W., Visser, A., van der Mei, H. C. and Bilkay, I. S. (2021). Candida Biofilm Formation Assay on Essential Oil Coated Silicone Rubber. Bio-protocol 11(5): e3941. DOI: 10.21769/BioProtoc.3941.
Category
Microbiology > Microbial biofilm > Response to antimicrobials
Biological Sciences > Biological techniques > Microbiology techniques
Do you have any questions about this protocol?
Post your question to gather feedback from the community. We will also invite the authors of this article to respond.
Share
Bluesky
X
Copy link










