- Submit a Protocol
- Receive Our Alerts
- Log in
- /
- Sign up
- My Bio Page
- Edit My Profile
- Change Password
- Log Out
- EN
- EN - English
- CN - 中文
- Protocols
- Articles and Issues
- For Authors
- About
- Become a Reviewer
- EN - English
- CN - 中文
- Home
- Protocols
- Articles and Issues
- For Authors
- About
- Become a Reviewer
In vitro Antigen-presentation Assay for Self- and Microbial-derived Antigens
Published: Vol 7, Iss 11, Jun 5, 2017 DOI: 10.21769/BioProtoc.2307 Views: 18541
Reviewed by: Andrea PuharGuangzhi ZhangAnonymous reviewer(s)

Protocol Collections
Comprehensive collections of detailed, peer-reviewed protocols focusing on specific topics
Related protocols
In Silico Prediction and In Vitro Validation of Bacterial Interactions in the Plant Rhizosphere Using a Synthetic Bacterial Community
Arijit Mukherjee [...] Sanjay Swarup
Nov 5, 2025 1655 Views
Dual Phospho-CyTOF Workflows for Comparative JAK/STAT Signaling Analysis in Human Cryopreserved PBMCs and Whole Blood
Ilyssa E. Ramos [...] James M. Cherry
Nov 20, 2025 2336 Views
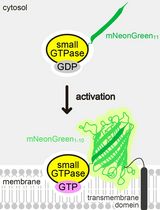
Detecting the Activation of Endogenous Small GTPases via Fluorescent Signals Utilizing a Split mNeonGreen: Small GTPase ActIvitY ANalyzing (SAIYAN) System
Miharu Maeda and Kota Saito
Jan 5, 2026 483 Views
Abstract
Antigen presenting cells (APC) are able to process and present to T cells antigens from different origins. This mechanism is highly regulated, in particular by Patter Recognition Receptor (PRR) signals. Here, I detail a protocol designed to assess in vitro the capacity of APC to present antigens derived from bacteria, apoptotic and infected apoptotic cells.
Keywords: Antigen presentationBackground
T cell lymphocytes express on their surface the T cell receptor (TCR), which allows the recognition of cellular (self) or microbial (non-self) antigens that are processed and presented as peptides bound to the major histocompatibility complex (MHC) molecules by antigen presenting cells (APC). APC are able to process antigens and to present them to T cells, and MHC-TCR interactions are critical steps for T cell activation during both infectious and autoimmune responses.
Previous works have described a mechanism of regulation of antigen presentation based on the stimulation of Pattern Recognition Receptors (PRRs), such as toll-like receptors (TLRs) (Blander and Medzhitov, 2004 and 2006). Indeed, TLR signals specifically from phagosomes containing microbial pathogens favor the presentation of non-self-antigens within MHC-II molecules. On the other hand, self-antigens generated after phagocytosis of apoptotic cells are directed to lysosomal degradation because of the absence of TLR stimuli. However, the segregation of self and non-self-antigens does not occur when both derive from infected apoptotic cells and are simultaneously carried by the same phagosome, which is optimally tailored by TLR signals for antigen presentation. Such mechanism of phagosome maturation and antigen presentation upon TLR triggering has been demonstrated in vitro using bone marrow derived dendritic cells (BMDC) and apoptotic murine B cells–either primary or A20 B cell line–previously incubated with the TLR4 ligand lipopolysaccharide (LPS), which is internalized by B cells and mimics bacterial infection (Blander and Medzhitov, 2004 and 2006; Campisi et al., 2016). Despite its elegance, this experimental system fails to reproduce bacterial invasion of the eukaryotic target cell. Furthermore, no T cell traceable antigens are present in the apoptotic cargo that internalized LPS.
I developed an in vitro alternative protocol where A20 cells are directly infected by the cell invasive bacteria Listeria monocytogenes expressing a recombinant antigen, allowing to assess the capacity of BMDC to present self and non-self-antigens derived from the same infected apoptotic cargo (Campisi et al., 2016).
Materials and Reagents
- Sterile pipette tips and serological pipettes (Fisher Scientific, FisherbrandTM)
- Optilux non-tissue culture10 cm Petri dishes (Corning, catalog number: 430591 )
- Sterile 50 and 15 ml conical tubes (Denville)
- 1 ml syringe with 26 G gauge needle (BD, catalog number: 309625 )
- 70 μm cell strainers (Fisher Scientific, FisherbrandTM, catalog number: 22-363-548 )
- Tissue culture 24 well plates (flat bottom) (Corning, Costar®, catalog number: 3524 )
- Tissue culture 96 well plates (flat bottom) (Corning, catalog number: 3595 )
- Sterile bacterial inoculating needles or loops
- Sterile 5 ml tubes with cap for bacterial culture (Corning, catalog number: 352058 )
- Tissue culture 6 well plates (flat bottom) (Corning, Costar®, catalog number: 3516 )
- 20 G gauge needle (BD, catalog number: 305175 )
- 3 ml syringe (BD, catalog number: 309656 )
- FACS tubes with rack (National Scientific, catalog number: TN0946-01R )
- Mice:
- Wild-type C57BL/6J mice
Note: We initially purchased them from THE JACKSON LABORATORIES and then bred in the mouse facility of the Icahn School of Medicine at Mount Sinai for at least 5 years. - OT-II TCR transgenic mice (strain B6.Cg-Tg(TcraTcrb)425Cbn/J) (THE JACKSON LABORATORIES, catalog number: 004194 ), which express the mouse alpha-chain and beta-chain T cell receptor that pairs with the CD4 coreceptor and is specific for an epitope derived from the chicken ovalbumin (OVA323-339) in the context of I-A b
- 1H3.1 TCR transgenic mice, which express the mouse alpha-chain and beta-chain T cell receptor that pairs with the CD4 coreceptor and is specific for the 52-68 fragment of the alpha-chain of I-E class II molecules (the Eα52-68 peptide) in the context of I-A b
- Antigen sources:
- Cell cargo: A20 cell line (ATCC, catalog number: TIB-208 )
- Bacteria: Listeria monocytogenes expressing ovalbumin (OVA) as a recombinant protein (Pope et al., 2001)
- Purified peptides: OVA329-337 (sequence ISQAVHAAHAEINEAGR) and Eα52-68 (sequence ASFEAQGALANIAVDKA)
- 70% ethanol
- 1x PBS (Sigma-Aldrich, catalog number: D8537 )
- Red blood cell lysis solution (Sigma-Aldrich, catalog number: R7757 )
- Bacterial growing medium: brain heart infusion (BHI) broth (BD, BactoTM, catalog number: 237500 )
- Ampicillin (Sigma-Aldrich, catalog number: A9393 )
- Anti-CD95 antibody, clone Jo2 (BD, BD Biosciences, catalog number: 554255 )
- Trypan blue stain (Thermo Fisher Scientific, GibcoTM, catalog number: 15250061 )
- Fetal bovine serum (FBS)
- EDTA disodium dihydrate (Biological Industries, BI, catalog number: 41-922 ), to dissolve in PBS at pH = 8, stock solution 0.5 M
- Penicillin-streptomycin (Thermo Fisher Scientific, GibcoTM, catalog number: 15140122 )
- Anti-CD4 magnetic microbeads for T cell positive selection (Miltenyi Biotec, catalog number: 130-049-201 )
- Carboxyfluorescein succinimidyl ester (CFSE) (Thermo Fisher Scientific, eBioscienceTM, catalog number: 65-0850-84 )
- Anti-mouse CD4-APC, clone RM4-5 (Thermo Fisher Scientific, eBioscienceTM, catalog number: 14-0042 )
- Optional: anti-mouse CD11c (clone N418), CD11b (clone M1/70) and MHC-II (clone M5/114.15.2) markers
- RPMI (Sigma-Aldrich, catalog number: R8758 )
- GM-CSF
Note: We used to prepare GM-CSF using J558 cells transfected with GM-CSF cDNA (Liu et al., 2006, p.148), but recombinant GM-CSF can be also purchased. - L-glutamine (Sigma-Aldrich, catalog number: G7513 )
- HEPES solution BioXtra, 1 M, pH 7.0-7.6 (Sigma-Aldrich, catalog number: H0887 )
- Sodium pyruvate (Sigma-Aldrich, catalog number: S8636 )
- MEM, nonessential amino acids (Sigma-Aldrich, catalog number: M7145 )
- β-mercaptoethanol (Sigma-Aldrich, catalog number: M6250 )
- IMDM (Sigma-Aldrich, catalog number: I3390 )
- Fc-block: rat anti-mouse CD16/32, clone 2.4G2 (BD, BD Biosciences, catalog number: 553141 )
- Sodium azide (NaN3) (Sigma-Aldrich, catalog number: 13412 )
Note: This product has been discontinued. - BMDC medium (see Recipes)
- A20 cell medium (see Recipes)
- T cell medium (see Recipes)
- FACS buffer (see Recipes)
Equipment
- Single channel pipettes, 1, 20, 200 and 1,000 μl
- Scissors
- Forceps
- Laminar flow hood
- Bench top centrifuge
- Hemocytometer or automatic cell counter
- Cell incubator (37 °C, 5% CO2)
- Bacterial incubator (37 °C) with shaker
- Sterile 100 ml Erlenmeyer flasks
- Flasks for cell culture
- Optical density (OD) reader
- MACS columns, LS columns (Miltenyi Biotec, catalog number: 130-042-401 )
- MACS separators
Note: I suggest QuadroMACS separator (Miltenyi Biotec, catalog number: 130-090-976 ) - Flow cytometer
Software
- Flow cytometer analysis software, FlowJo, LLC
Procedure
- Bone marrow isolation and dendritic cell differentiation and culture
- Sacrifice mice using CO2 accordingly to the institutional IACUC recommendations.
- Spray the entire mouse fur with 70% ethanol to avoid contaminations.
- Using a scissor cut the fur at the hip area and pull the skin down off the leg toward the foot.
- Once the skin removed, cut into pelvis and remove tibia and femur using a scissor.
- Hold tibia and femur with forceps and clean bones by cutting off all muscle/fat tissue using a scissor.
- Place the cleaned bones under a laminar flow hood -to work aseptically- into a 10 cm Petri dish with ice cold sterile PBS.
- Fill 1 ml syringe with fresh sterile cold PBS and, by holding the bone with the forceps, insert the needle into one hand and flush the bone marrow out the other hand in a second Petri dish containing 2-3 ml sterile cold PBS.
- Make a single cell suspension by passing through up and down with the same syringe.
- Refill the syringe with the PBS from the second Petri dish and repeat steps A6 and A7 until the bone becomes clear.
- Collect the cells in a conical 50 ml tube by filtering through a 70 μm cell strainer to remove any contamination of bone debris and tissue. Wash the Petri dish by pipetting up and down 1-2 ml PBS to be sure to recover all bone marrow cells, and add to the 50 ml tube through the 70 μm cell strainer.
- Adjust the final volume of the conical 50 ml tube to 30-40 ml with ice cold PBS.
- Pellet cells for 5 min at 435 x g.
- Remove the supernatant and resuspend in 1 ml of red blood cell lysis buffer, incubate for 1 min at room temperature, then add 25 ml of PBS to wash the cells and centrifuge for 5 min at 435 x g.
- Resuspend the pellet in 5 ml of Bone Marrow Dendritic Cells (BMDC) medium (see Recipes) and filter in a new 50 ml conical tube using a clean 70 μm cell strainer to remove dead cells. Count the cells using a hemocytometer or an automatic cell counter. Typically from 1 adult mouse 10 week old the yield should be 40 x 106 cells.
- Adjust the volume to a density of 106 cells/ml using BMDC medium, and plate 1 ml per well in a 24 well tissue culture plate.
- Incubate for 5 days in a cell incubator (37 °C, 5% CO2), adding 1 ml of BMDC medium at day 3 of culture. This is day 0. BMDC are semi-adherent, round cells that should not show extending dendrites when immature. BMDC purity can be assessed by flow cytometry using anti-mouse CD11c and MHC-II markers.
- Before use, count cells from 1 well after removing BMDC by pipetting up and down the medium very gently and washing out the well with 1 ml ice cold PBS. This cell number should be constant throughout the 24 wells. Centrifuge for 5 min at 279 x g.
- Add directly to the BMDC culture the phagocytic cargo (see Procedure B) resuspended in 200 μl of PBS or medium and then centrifuge the 24 well plate at 279 x g for 2 min.
- Alternatively, to get rid of contaminant cells that are not differentiated BMDC and adhere to the plate, BMDC can be removed from the 24 well plate as described in step A12 and replated in a new plate.
- Incubate BMDC (replated or not) with the phagocytic cargos for 8 h.
- Leave some BMDC without phagocytic cargo to be pulsed with peptide controls (see step A17 below).
- Harvest BMDC, collect in a conical tube and wash with cold PBS.
- Centrifuge for 5 min at 279 x g.
- Resuspend in T cell medium (see Recipes) at the concentration of 106 cells/ml.
- Plate in a 96 well plate 100 μl of BMDC immediately before adding the T cells. Pulsed unstimulated BMDC with 1 μg/ml of OVA329-337 and, in separate wells, Eα52-68 peptides. BMDC can be left on ice until T cells are ready.
- Sacrifice mice using CO2 accordingly to the institutional IACUC recommendations.
- Phagocytic cargo preparation
- Listeria monocytogenes culture
- The night before the infection, prepare a bacteria pre-culture: aseptically pick a loopful of frozen bacteria from the stock using a needle or loop and inoculate into a 5 ml tube with 3 ml of BHI medium.
- Incubate for 16 h in a 37 °C incubator shaker at 250 rpm.
- The next day, dilute the overnight culture 1/20 in a sterile flask with 20 ml of fresh BHI medium. Cap and incubate in a 37 °C incubator shaker until the culture reaches the exponential phase (0.5 < OD600 < 1) (usually it takes 1 h). Determine the bacterial concentration (for Listeria monocytogenes, an OD600 = 1 corresponds to 5 x 108 bacteria/ml) and calculate the volume of culture needed to infect A20 cells and BMDC at a multiplicity of infection (moi) of 100.
- Transfer the appropriate volume of bacterial culture in one or more 50 ml tubes, centrifuge for 10 min at 3,113 x g, wash twice with sterile PBS.
- Add to cells 200 μl of bacteria in PBS or BMDC medium per well of cell culture.
Note: Before addition to BMDC, bacteria should be killed by incubation for 2 h at 37 °C in PBS containing 50 μl of ampicillin, while A20 cells are infected with live bacteria.
- The night before the infection, prepare a bacteria pre-culture: aseptically pick a loopful of frozen bacteria from the stock using a needle or loop and inoculate into a 5 ml tube with 3 ml of BHI medium.
- Preparation of A20 cells as apoptotic cell cargo
- A20 cells are grown in small flasks in A20 cell medium (see Recipes) in a cell incubator at 37 °C with 5% CO2.
- Three days before the assay, remove the A20 cells from the flask by pipetting up and down and transfer in a 50 ml conical tube.
- Count A20 cells, centrifuge at 279 x g for 5 min and resuspend them in fresh medium at 1 x 106 cells/ml.
- Plate 3 ml of cells per well in 6 well plates and place in the incubator.
- Induction of apoptosis in A20 cells:
A20 cells will be rendered apoptotic by anti-CD95 (FasR) treatment, with or without previous bacteria infection, and then used as plain (= uninfected) or infected apoptotic cargos.- Plain apoptotic cells:
At day 5, remove and count A20 cells, centrifuge at 279 x g for 5 min, then resuspend and plate 3 ml in a 6 well plate at 1 x 106 cells/ml in fresh medium containing the anti-CD95 at the final concentration of 0.5 μg/ml.
Incubate for 2 h in a cell incubator. The duration of anti-CD95 treatment can vary and should be precisely determined by each investigator. Apoptosis can be verified by flow cytometry after 7ADD and Annexin V staining (apoptotic cells should be Annexin V positive and 7ADD negative). - Infected apoptotic cells
At day 5, remove and count A20 cells, centrifuge at 279 x g for 5 min, then resuspend and plate 3 ml in a 6 well plate at 1 x 106 cells/ml in fresh medium. Add 200 μl of Listeria at a moi = 100. Incubate for 8 h in a cell incubator.
After 8 h, add ampicillin at the final concentration of 50 μg/ml (to kill all the bacteria) and 0.5 μg/ml of anti-CD95 to the culture, cultivate for additional 2 h.
- Plain apoptotic cells:
- Harvest and count apoptotic cells (they should not appear blue after trypan blue staining–more than 90% must be trypan blue negative–if they are, they cannot be used for the assay and the investigator should re-work the duration of the anti-CD95 treatment).
- Centrifuge at 279 x g for 5 min, and resuspend in 200 μl PBS or medium per well.
- Apoptotic cells are added immediately to the BMDC culture at a ratio of 1:2 (BMDC:apoptotic cells) for 8 h.
- A20 cells are grown in small flasks in A20 cell medium (see Recipes) in a cell incubator at 37 °C with 5% CO2.
- Listeria monocytogenes culture
- CD4 T cell isolation and CFSE labeling
- Harvest spleens and prepare a cell suspension in a 10 cm Petri dish containing 5 ml cold PBS by pressing the tissue through a 70 μm cell strainer followed by homogenization using a 20 G needle and a 3 ml syringe. Make a single cell suspension by passing through up and down with the same syringe. Typically, one mouse spleen contains 1 x 108 splenocytes.
- Transfer the cell suspension in a 15 ml conical tube and centrifuge for 5 min at 435 x g.
- Optional: Remove the supernatant and resuspend in 1 ml of red blood lysis buffer, incubate for 1 min at room temperature, then add 13 ml of PBS to wash the cell and centrifuge for 5 min at 435 x g. This step can be skipped since red blood cells are eliminated during the step of CD4+ T cell positive selection.
- Incubate splenocytes in 1x PBS containing 1 μg/ml anti-Fc receptor, 2% FBS, 2 mM EDTA, 100 μg/ml penicillin, 100 μg/ml streptomycin and the anti-CD4 magnetic microbeads for CD4 T cell positive selection (Miltenyi Biotec), according to the manufacturer’s instructions.
- Proceed to CD4+ T cell positive selection by magnetic columns (Miltenyi Biotec), according to the manufacturer's instructions.
- Count and resuspend purified CD4 T cells in PBS at the concentration of 2 x 106 cells/ml.
- Add CFSE (final concentration 2.5 μM) very slowly to the cells while vortexing the tubes gently. Incubate for 10 min at 37 °C in the dark.
Note: Leave some CD4 T cells unstained to perform flow cytometry compensations. - Wash twice with PBS by completely filling the tube and centrifuging for 5 min at 435 x g. Successful CFSE staining of the cells should give a yellow/green pellet.
- Resuspend cells in T cell medium at the concentration of 2 x 106 cells/ml.
- Add 100 μl of CD4 T cells to the 96 well plates where BMDC were previously plated.
Note: OT-II and 1H3.1 TCR transgenic CD4 T cells should be plated in separate wells to avoid antigen competition. - Co-culture CD4 T cells and BMDC for 5 days.
- Harvest spleens and prepare a cell suspension in a 10 cm Petri dish containing 5 ml cold PBS by pressing the tissue through a 70 μm cell strainer followed by homogenization using a 20 G needle and a 3 ml syringe. Make a single cell suspension by passing through up and down with the same syringe. Typically, one mouse spleen contains 1 x 108 splenocytes.
- Assessing antigen presentation
- At day 5, wash twice the plate containing the co-culture of CD4 T cells and BMDC with 200 μl of FACS buffer (see Recipes) by centrifuging for 2 min at 778 x g. Discard the supernatant.
- Add 100 μl of anti-mouse CD4 (1/100) in FACS buffer and incubate for 20 min on ice in the dark.
- Wash twice with 200 μl of FACS buffer.
- Resuspend in 200 μl of FACS buffer and analyze by flow cytometry.
- At day 5, wash twice the plate containing the co-culture of CD4 T cells and BMDC with 200 μl of FACS buffer (see Recipes) by centrifuging for 2 min at 778 x g. Discard the supernatant.
Data analysis
The following conditions should be prepared (at least in duplicate):
- OT-II CD4 T cells + BMDC that phagocytized plain apoptotic A20 cells = no T cell proliferation.
- OT-II CD4 T cells + BMDC that phagocytized Listeria-OVA infected apoptotic A20 cells = T cell proliferation.
- OT-II CD4 T cells + BMDC infected with Listeria-OVA = T cell proliferation.
- OT-II CD4 T cells + BMDC pulsed with OVA329-337 = positive control for OT-II CD4 T cell proliferation.
- OT-II CD4 T cells + BMDC pulsed with Eα52-68 peptide = negative control for OT-II CD4 T cell proliferation.
- 1H3.1 CD4 T cells + BMDC that phagocytized plain apoptotic A20 cells = no proliferation.
- 1H3.1 CD4 T cells + BMDC that phagocytized Listeria-OVA infected apoptotic A20 cells = T cell proliferation.
- 1H3.1 CD4 T cells + BMDC infected with Listeria-OVA = no T cell proliferation.
- 1H3.1 CD4 T cells + BMDC pulsed with OVA329-337 = negative control for 1H3.1 CD4 T cell proliferation.
- 1H3.1 CD4 T cells + BMDC pulsed with Eα52-68 peptide = positive control for 1H3.1 CD4 T cell proliferation.
- A20 cells are a Balb/c-derived B cell line that expresses I-E class II molecules. After phagocytosis of infected apoptotic A20 cells, the simultaneous compartmentalization of microbial and apoptotic cargo allows BMDC to process and present both the bacteria-derived antigen OVA329-337 and the cell-derived antigen Eα52-68, inducing the proliferation of OT-II and 1H3.1 CD4 T cells. On the other hand, in the absence of infection and TLR stimulus, antigens from plain apoptotic cells fail to be presented and no proliferation of 1H3.1 CD4 T cells should be observed (Figure 1).

Figure 1. Regulation of antigen presentation by TLR activation. In this protocol, antigen presentation is assessed through proliferation of antigen-specific CD4 T cells diluting the CFSE after 5 days of incubation with antigen presenting cells (APC, here bone marrow derived dendritic cells), which phagocytized plain (A) or infected (C) apoptotic cells, or that have been infected with the bacteria Listeria monocytogenes expressing the recombinant protein ovalbumin (OVA) (B). I use as apoptotic cargos the A20 cell line, which expresses the Balb/c-derived Eα52-68 antigen recognized by TCR transgenic 1H3.1 CD4 T cells. OVA329-337 antigen derived from recombinant bacteria Listeria-monocytogenes is recognized by TCR transgenic OT-II CD4 T cells as microbial antigen. - As shown in the Figure 1, phagocytosis of apoptotic cells is followed by lysosomal degradation of the cargo and no antigen presentation occurs (Figure 1A), while during bacterial infection TLR activation promotes phagosome maturation for optimal microbial antigen presentation (Figure 1B). When apoptotic cells are infected, both apoptotic and microbial cargos are found in the same phagosome where the presence of TLR signals favors antigen presentation of both self- and bacterial derived-antigens (Figure 1C).
Notes
- One mouse per strain (C57BL/6J, OT-II and 1H3.1 TCR transgenic) should give enough cells to perform the entire experiment.
- We observed down-regulation of the CD3 after antigen stimulation, thus an anti-CD3 staining is not necessary. For flow cytometry analysis, simply gate on live CD4+ T cells. This gating strategy is also enough to exclude BMDC. Alternatively, you can stain BMDC using anti-mouse CD11c and CD11b markers.
- Alternative versions of this protocol can be found in Blander and Medzhitov (2006) and Nair-Gupta et al. (2014). The latter paper describes in vitro antigen presentation assays in the context of CD8 T cells.
Recipes
- BMDC medium
Complete RPMI with 10 ng/ml of GM-CSF and 5% FBS, plus 100 μg/ml penicillin, 100 μg/ml streptomycin, 2 mM L-glutamine, 10 mM HEPES, 1 nM sodium pyruvate, 1x MEM nonessential amino acids, and 2.5 μM β-mercaptoethanol - A20 cell medium
Complete RPMI with 10% FBS, plus 100 μg/ml penicillin, 100 μg/ml streptomycin, 2 mM L-glutamine, 10 mM HEPES, 1 nM sodium pyruvate, 1x MEM nonessential amino acids, and 2.5 μM β-mercaptoethanol - T cell medium
Complete IMDM with 10% FBS, plus 100 μg/ml penicillin, 100 μg/ml streptomycin, 2 mM L-glutamine, 10 mM HEPES, 1 nM sodium pyruvate, 1x MEM nonessential amino acids, and 2.5 μM β-mercaptoethanol - FACS buffer
1x PBS with 2% FBS, plus 1 μg/ml Fc block and 0.1% NaN3
Acknowledgments
L.C. was supported by an Arthritis Foundation Research Fellowship Award. The protocol described herein was based on the paper Campisi et al. (2016). L.C. thanks Ivan Marazzi for advise and support. 1H3.1 TCR transgenic mice used in the paper Campisi et al. (2016) were a kind gift from Adrian Morelli to J. Blander’s laboratory under material transfer agreement (MTA).
The author declares no conflict of interest.
References
- Blander, J. M. and Medzhitov, R. (2004). Regulation of phagosome maturation by signals from toll-like receptors. Science 304(5673): 1014-1018.
- Blander, J. M. and Medzhitov, R. (2006). Toll-dependent selection of microbial antigens for presentation by dendritic cells. Nature 440(7085): 808-812.
- Campisi, L., Barbet, G., Ding, Y., Esplugues, E., Flavell, R. A. and Blander, J. M. (2016). Apoptosis in response to microbial infection induces autoreactive TH17 cells. Nat Immunol 17(9): 1084-1092.
- Liu, K., Charalambous, A. and Steinman, R. M., (2006). Some biological features of dendritic cells in mouse. In: Fox, J., Barthold, S., Davisson, M., Newcomer, C., Quimby, F. and Smith, A. (Eds.). The Mouse in Biomedical Research. Academic Press, pp: 135-249.
- Nair-Gupta, P., Baccarini, A., Tung, N., Seyffer, F., Florey, O., Huang, Y., Banerjee, M., Overholtzer, M., Roche, P. A., Tampe, R., Brown, B. D., Amsen, D., Whiteheart, S. W. and Blander, J. M. (2014). TLR signals induce phagosomal MHC-I delivery from the endosomal recycling compartment to allow cross-presentation. Cell 158(3): 506-521.
- Pope, C., Kim, S. K., Marzo, A., Masopust, D., Williams, K., Jiang, J., Shen, H. and Lefrançois, L. (2001). Organ-specific regulation of the CD8 T cell response to Listeria monocytogenes infection. J Immunol 166(5): 3402-9.
Article Information
Copyright
© 2017 The Authors; exclusive licensee Bio-protocol LLC.
How to cite
Campisi, L. (2017). In vitro Antigen-presentation Assay for Self- and Microbial-derived Antigens. Bio-protocol 7(11): e2307. DOI: 10.21769/BioProtoc.2307.
Category
Immunology > Immune cell function > Antigen-specific response
Microbiology > Microbe-host interactions > Bacterium
Cell Biology > Cell signaling > Intracellular Signaling
Do you have any questions about this protocol?
Post your question to gather feedback from the community. We will also invite the authors of this article to respond.
Share
Bluesky
X
Copy link