- Submit a Protocol
- Receive Our Alerts
- Log in
- /
- Sign up
- My Bio Page
- Edit My Profile
- Change Password
- Log Out
- EN
- EN - English
- CN - 中文
- Protocols
- Articles and Issues
- For Authors
- About
- Become a Reviewer
- EN - English
- CN - 中文
- Home
- Protocols
- Articles and Issues
- For Authors
- About
- Become a Reviewer
Construction of Human Monocyte Derived Macrophages Armed with Oncolytic Viruses
Published: Vol 3, Iss 13, Jul 5, 2013 DOI: 10.21769/BioProtoc.809 Views: 10032

Protocol Collections
Comprehensive collections of detailed, peer-reviewed protocols focusing on specific topics
Related protocols
Human Blood Component Vaccinia Virus Neutralization Assay
Laura Evgin and John Bell
Dec 5, 2015 9365 Views
Selective Enrichment and Identification of Cerebrospinal Fluid-Contacting Neurons In Vitro via PKD2L1 Promoter-Driven Lentiviral System
Wei Tan [...] Qing Li
Nov 20, 2025 1335 Views
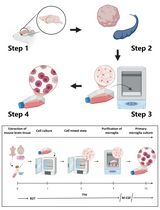
Revisiting Primary Microglia Isolation Protocol: An Improved Method for Microglia Extraction
Jianwei Li [...] Guohui Lu
Dec 5, 2025 1460 Views
Abstract
Macrophages are involved in many key physiological processes and complex responses such as inflammatory, immunological, infectious and neoplastic diseases. The appearance and activation of macrophages are thought to be rapid events in the development of many pathological lesions, including malignant tumours, atherosclerotic plaques, and arthritic joints. This has prompted recent attempts to use macrophages as novel cellular vehicles for gene therapy, in which macrophages are genetically modified ex vivo and then reintroduced into the body with the hope that a proportion will then home to the diseased site. Here, we describe a protocol for preparing monocyte-derived macrophages (MDM) and arming these with oncolytic viruses (OV) as a novel way for delivering anti-cancer therapies. In this approach, proliferation of macrophages co-transduced with a hypoxia-regulated E1A/B construct and an E1A-dependent oncolytic adenovirus, is restricted to prostate tumour cells using prostate-specific promoter elements from the TARP, PSA, and PMSA genes (Muthana et al., 2013; Muthana et al., 2011). When such co-transduced cells reach an area of extreme hypoxia (like that found in tumours), the E1A/B proteins are expressed, thereby activating replication of the adenovirus. The virus is subsequently released by the host macrophage and infects neighboring tumour cells. The virus then infects neighboring cells but only proliferates and is cytotoxic in prostate tumour cells. OV kill cancer cells by a number of mechanisms, including direct lysis, apoptosis, autophagy and shutdown of protein synthesis, as well as the induction of anti-tumoural immunity. Using macrophages to deliver OV ensures that they are protected from the many hazards they face in circulation including neutralizing antibodies, complement activation and non-specific uptake by other tissues such as the liver and spleen.
Materials and Reagents
- Blood (Sheffield Blood Transfusion Service)
- 50 ml falcon tubes (BD Biosciences, Falcon®, catalog number: 734-0451 )
- Hank's Balanced Salt Solution (HBSS) (without Calcium, Ca2+ and Magnesium, Mg2+) (Lonza BioWhittaker Ltd., catalog number: 10-543Q )
- Ficoll-Hypaque (GE Healthcare, catalog number: 17-1440-02 )
- IMDM medium (Lonza BioWhittaker Ltd., catalog number: 12-722 )
- Human AB serum (Lonza BioWhittaker Ltd., Wokingham, UK)
- L-Glutamine (Lonza BioWhittaker Ltd., catalog number: 17-605 )
- RPMI medium (Lonza BioWhittaker Ltd., catalog number: 12-115 )
- Fetal bovine serum (FBS) (Biosera, catalog number: FB-1000 )
- Phosphate buffered saline (PBS) (Lonza BioWhittaker Ltd., catalog number: 17-516F )
- Trypsin/EDTA (Promocell Ltd., catalog number: C-41000 )
- Adenoviruses (Adenoviruses used in our experiment include AdCMV-GFP, and oncolytic Ad[1/PPTE1A]) (kind gift from professor Magnus Essand, Uppsala, Sweden)
- Hypoxia driven plasmid (HRE-E1A/B)
- Macrophage Amaxa Nucleofector® kit (Lonza BioWhittaker Ltd.)
Equipment
- T75 tissue culture flask (BD Biosciences, Falcon®)
- 12-well plate (BD Biosciences, Falcon®, catalog number: 734-2324 )
- Centrifuge (MSE Mistral 2000R)
- Haemocytometer (Camlab Limited, catalog number: 1127884 )
- Nucleofector® machine (Lonza BioWhittaker Ltd.)
Procedure
- Monocyte Isolation
- Venous blood collected by Sheffield Teaching Hospitals (STH) blood bank was collected from healthy donors and consolidated into one bag of waste buffy coat.
- 25 ml of this blood was poured into 50 ml Falcon tubes and then filled up to the 40 ml line with 15 ml of HBSS (without Calcium, Ca2+ and Magnesium, Mg2+).
- The tubes were then spun at 1,200 x g for 20 min (4 °C and Brake Rate of 0).
- After spinning, the cloudy white blood cell layer (below the plasma) was removed by pipette and collecting the transferred into two new 50 ml Falcon tubes where it was made up to 30 ml with HBSS (w/o Ca2+/Mg2+).
- The 30 ml of white cells were then carefully layered on top of 20 ml of Ficoll-Hypaque (in 50 ml Falcon tubes).
- These tubes were then placed in the centrifuge and once again spun at 1,200 x g (4 °C and Brake Rate of 0) for 20 min.
- Once again, the cloudy white cell layer was removed and made up to 40 ml with HBSS (w/o Ca2+/Mg2+) in a new 50 ml Falcon tube.
- This tube was then spun at 400 x g for 5 min (4 °C and Brake Rate of 3) to wash and pellet the cells.
- This process was repeated three times.
- The cells were then counted using a haemocytometer and diluted with IMDM (supplemented with 2% Human AB serum and 4 mM L-Glutamine) so that there were 5-7 x 106 cells /ml.
- To plate the cells down 1 ml of this cell suspension was added to each T75 (BD falcon-these flasks are superior when it comes to infecting with virus) flask and topped up to 10 ml with supplemented IMDM. The cells were then incubated for two hours (37 °C, 5% CO2). After two hours the flasks were washed with HBSS to remove the non-adherent cells and then refilled with 10 ml of supplemented IMDM.
- Venous blood collected by Sheffield Teaching Hospitals (STH) blood bank was collected from healthy donors and consolidated into one bag of waste buffy coat.
- Subculture of monocytes and differentiation into monocyte derived macrophages (MDM)
Monocytes isolated as above and cultured in 10 ml of IMDM, supplemented with L-glutamine (4 mM) and Human AB serum (2%), for the first 24 h. After this point the medium was replaced with 5 ml of RPMI, supplemented with L-glutamine (4 mM) and 10% FBS. Medium was replaced every three days depending on which other procedures were performed and monocyte derived MDM. Macrophages are visible after 24 hours these have a different morphology to monocytes, which are non-adherent and spherical. Macrophages on the other hand are larger and have irregular features. The can possess dendrites and appear spindle shaped. - Co-transduction of MDM
MDM were co-transduced with a therapeutic oncolytic adenovirus and a hypoxia-regulated plasmid carrying the replication component of the virus E1A. A description of the virus and plasmid can be found in (Muthana et al., 2013; Muthana et al., 2011).
Note: The adenoviruses used in this study include AdCMV-GFP, and oncolytic Ad[1/PPTE1A].- MDM infection with human adenovirus
- The plated monocytes were washed the following day with HBSS and re-suspended in 5 ml of RPMI (supplemented with 10% FBS and L-Glutamine). This prevents the virus binding to the Human AB serum in the IMDM and neutralising the viral particles.
- The viral particles were added at a multiplicity of infection (MOI) 100 and placed in the incubator over-night.
- After an overnight incubation the cells were washed in PBS and fresh supplemented RPMI medium was added. Virus infection was assessed by flow cytometry and fluorescent microscopy for expression of green fluorescent protein (GFP) reporter gene.
- The plated monocytes were washed the following day with HBSS and re-suspended in 5 ml of RPMI (supplemented with 10% FBS and L-Glutamine). This prevents the virus binding to the Human AB serum in the IMDM and neutralising the viral particles.
- Transfection of MDM using Amaxa Nucleofection
- 24 h later infected macrophages were harvested using trysin/EDTA and then transfected with a hypoxia driven plasmid (HRE-E1A/B) using the macrophage Amaxa Nucleofector® kit. This was carried out according to the manufacturer’s protocol. In brief, RPMI (1.5 ml) supplemented with 10% FCS and L-glutamine was added to the wells of a 12-well plate and pre-incubated at 37 °C.
- Three-day-old MDM were trypsinised, centrifuged at 400 x g for 5 min (at room temperature) and resuspended at 8 x 105 cells/ ml. The supernatant was completely discarded and 100 μl of Amaxa Nucleofector® solution added as well as 3 μg plasmid (HRE-E1A/B). The cell suspension was then inserted into the Nucleofector® machine and the Y-10 program selected. Once the machine displayed “OK”, the sample was removed, 500 μl of pre-warmed RPMI supplemented with 10% FCS and L-glutamine was added and the entire cell suspension was transferred to the appropriately labelled well. The 12-well plate was then incubated for 24 h. Plasmid transfection was optimised using the pmaxGFP plasmid supplied with the kit according to the manufacturer’s protocol. In brief, GFP expression was assessed 24-48 h after transfection by fluorescent microscopy and flow cytometry.
- Co-transduced macrophages can be delivered to tumour cells in vitro (e.g. 3D tumour spheroids) or intravenously to tumour bearing mice. Tumour cell death as a result of the OV killing can be determined.
- 24 h later infected macrophages were harvested using trysin/EDTA and then transfected with a hypoxia driven plasmid (HRE-E1A/B) using the macrophage Amaxa Nucleofector® kit. This was carried out according to the manufacturer’s protocol. In brief, RPMI (1.5 ml) supplemented with 10% FCS and L-glutamine was added to the wells of a 12-well plate and pre-incubated at 37 °C.
- MDM infection with human adenovirus
Acknowledgments
This protocol is adapted from Muthana et al. (2011) and Muthana et al. (2013).
References
- Muthana, M., Rodrigues, S., Chen, Y. Y., Welford, A., Hughes, R., Tazzyman, S., Essand, M., Morrow, F. and Lewis, C. E. (2013). Macrophage delivery of an oncolytic virus abolishes tumor regrowth and metastasis after chemotherapy or irradiation. Cancer Res 73(2): 490-495.
- Muthana, M., Giannoudis, A., Scott, S. D., Fang, H. Y., Coffelt, S. B., Morrow, F. J., Murdoch, C., Burton, J., Cross, N., Burke, B., Mistry, R., Hamdy, F., Brown, N. J., Georgopoulos, L., Hoskin, P., Essand, M., Lewis, C. E. and Maitland, N. J. (2011). Use of macrophages to target therapeutic adenovirus to human prostate tumors. Cancer Res 71(5): 1805-1815.
Article Information
Copyright
© 2013 The Authors; exclusive licensee Bio-protocol LLC.
How to cite
Muthana, M., Richardson, J., Rodrigues, S. and Lewis, C. (2013). Construction of Human Monocyte Derived Macrophages Armed with Oncolytic Viruses. Bio-protocol 3(13): e809. DOI: 10.21769/BioProtoc.809.
Category
Cancer Biology > Tumor immunology > Cancer therapy > Cell isolation and culture
Cell Biology > Cell isolation and culture > Cell isolation
Immunology > Immune cell function > Macrophage
Do you have any questions about this protocol?
Post your question to gather feedback from the community. We will also invite the authors of this article to respond.
Share
Bluesky
X
Copy link










